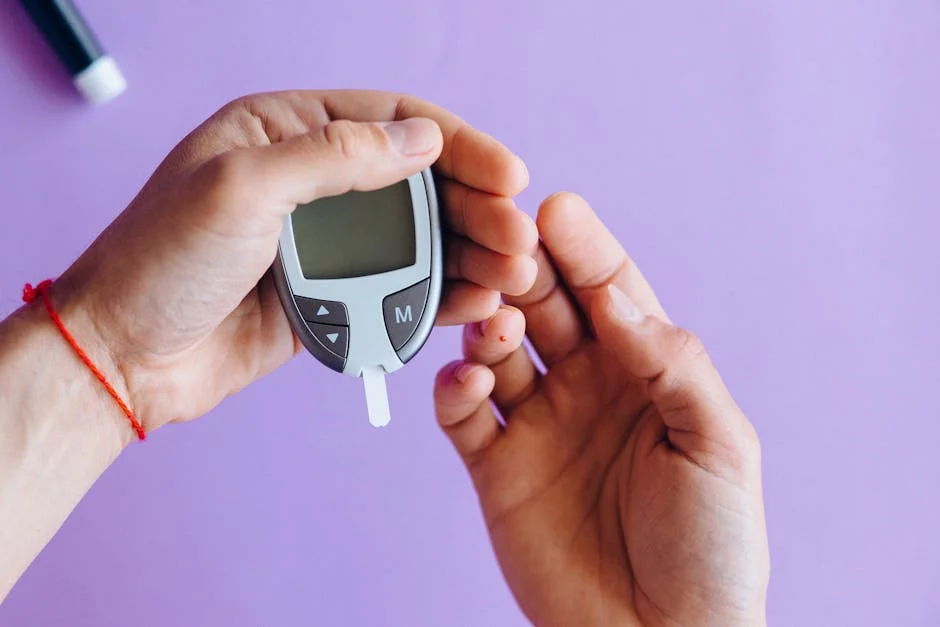
The fasting sugar test is one of the most widely used screening tools for checking blood glucose levels after a period without food. Because it measures glucose when the body is not actively processing a recent meal, it offers a clearer snapshot of baseline blood sugar regulation than many random checks. Clinicians often rely on this fasting glucose measurement to identify early trends toward insulin resistance, prediabetes, or diabetes, and it can also be used to monitor how well a treatment plan is working. The idea is straightforward: you fast for a set number of hours, usually overnight, and a blood sample is taken in the morning. Yet the meaning behind the number can be complex, influenced by hormones, sleep, stress, medications, and underlying metabolic health. Understanding how the test works and what it can—and cannot—tell you helps you use the result wisely rather than reacting to a single reading in isolation.
Table of Contents
- My Personal Experience
- Understanding the Fasting Sugar Test and Why It Matters
- How the Fasting Sugar Test Works in the Body
- Who Should Consider Getting a Fasting Sugar Test
- How to Prepare Correctly for Accurate Results
- What the Numbers Mean: Typical Ranges and Interpretation
- Fasting Sugar Test vs A1C vs Oral Glucose Tolerance
- Factors That Can Skew a Fasting Sugar Test Result
- Expert Insight
- What to Expect During the Test and Afterward
- Improving Fasting Glucose Through Lifestyle Changes
- Medical Next Steps When Results Are High
- Using Home Monitoring to Complement a Fasting Sugar Test
- Common Mistakes to Avoid Before and After Testing
- Long-Term Tracking and What a Healthy Trend Looks Like
- Watch the demonstration video
- Frequently Asked Questions
- Trusted External Sources
My Personal Experience
I had to do a fasting sugar test last month after my annual checkup showed my blood sugar was a little higher than usual. The night before, I stopped eating after dinner and set a reminder so I wouldn’t mindlessly snack while watching TV. By morning I was hungrier than I expected and had a slight headache, but I stuck to plain water and skipped my usual coffee. At the lab, they took my blood pretty quickly, and the hardest part was honestly just sitting there feeling a bit shaky and impatient. Once I finally ate breakfast afterward, I felt normal again within minutes. Waiting for the results made me more anxious than the test itself, but it also pushed me to pay closer attention to what I’m eating day to day.
Understanding the Fasting Sugar Test and Why It Matters
The fasting sugar test is one of the most widely used screening tools for checking blood glucose levels after a period without food. Because it measures glucose when the body is not actively processing a recent meal, it offers a clearer snapshot of baseline blood sugar regulation than many random checks. Clinicians often rely on this fasting glucose measurement to identify early trends toward insulin resistance, prediabetes, or diabetes, and it can also be used to monitor how well a treatment plan is working. The idea is straightforward: you fast for a set number of hours, usually overnight, and a blood sample is taken in the morning. Yet the meaning behind the number can be complex, influenced by hormones, sleep, stress, medications, and underlying metabolic health. Understanding how the test works and what it can—and cannot—tell you helps you use the result wisely rather than reacting to a single reading in isolation.
Blood glucose is tightly regulated by a balance of insulin production, insulin sensitivity, liver glucose output, and counter-regulatory hormones such as cortisol and glucagon. A fasting glucose test is especially useful because it reduces the immediate impact of food, allowing the body’s internal glucose management to be assessed with fewer variables. That said, “fasting” doesn’t mean the body is inactive; overnight, the liver releases glucose to keep the brain and essential organs fueled. If insulin response is impaired or if the liver is producing more glucose than needed, fasting levels can rise. For some people, a normal fasting result can still coexist with abnormal post-meal spikes, while others have elevated fasting numbers due to increased liver output even before meals. For that reason, the fasting sugar test is often interpreted alongside other markers like A1C, postprandial readings, or an oral glucose tolerance test, depending on symptoms and risk factors.
How the Fasting Sugar Test Works in the Body
During fasting, the body transitions from using dietary carbohydrates to relying on stored energy. After several hours without food, insulin levels generally decrease, and the liver begins releasing glucose through glycogenolysis (breaking down glycogen) and, later, gluconeogenesis (producing glucose from non-carbohydrate sources). A fasting blood sugar test captures the outcome of this balance: how much glucose is circulating and how effectively insulin keeps it in range. In a metabolically healthy person, fasting glucose remains relatively stable because insulin sensitivity is adequate and the liver’s output is properly restrained. When insulin resistance develops, the pancreas may need to release more insulin to keep fasting glucose normal. Over time, if the pancreas cannot keep up, fasting levels can rise, which is why elevated fasting results can be an early warning sign even before symptoms appear. If you’re looking for fasting sugar test, this is your best choice.
It’s also important to recognize the role of hormones that naturally rise in the morning. Cortisol and growth hormone can increase glucose availability to prepare the body for waking activity. This physiologic shift can contribute to the “dawn phenomenon,” where morning glucose is higher than expected, especially in people with diabetes or prediabetes. Because the fasting sugar test is often done in the morning, these hormonal patterns can influence results. Sleep deprivation, acute illness, and high stress can further increase cortisol and adrenaline, sometimes causing a higher fasting reading. Conversely, prolonged fasting beyond the recommended window can sometimes lower glucose in certain individuals or trigger counter-regulatory hormone responses that raise it. Understanding these mechanics helps explain why preparation and timing matter, and why repeating the test or pairing it with other measures can provide a more reliable picture than a single number.
Who Should Consider Getting a Fasting Sugar Test
A fasting sugar test can be helpful for many groups, not only those already diagnosed with diabetes. People with a family history of type 2 diabetes, a history of gestational diabetes, polycystic ovary syndrome (PCOS), high blood pressure, abnormal cholesterol or triglycerides, fatty liver disease, or central weight gain often have higher risk of insulin resistance. For these individuals, a fasting glucose test may serve as an early checkpoint to detect changes before complications develop. Some people seek testing because of symptoms that could be related to blood sugar swings, such as increased thirst, frequent urination, unexplained fatigue, blurred vision, slow wound healing, or recurrent infections. Even when symptoms are mild or intermittent, a fasting measurement can support a broader evaluation when combined with clinical history and other lab results.
Screening can also be relevant for people who appear “healthy” by weight or fitness standards but have risk factors like a strong genetic predisposition, a sedentary job, chronic sleep disruption, or a diet high in refined carbohydrates and sugary beverages. Metabolic risk is not determined by appearance alone; visceral fat, muscle mass, and liver fat can influence insulin sensitivity in ways that aren’t obvious from the scale. Additionally, certain medications—such as steroids, some antipsychotics, and specific immunosuppressants—can raise glucose levels and may warrant periodic monitoring. Pregnant individuals are typically screened with other protocols, but fasting values may still be evaluated depending on local guidelines. Ultimately, deciding when to test should be individualized, but for many adults, periodic fasting glucose testing is a practical, accessible way to track metabolic health over time. If you’re looking for fasting sugar test, this is your best choice.
How to Prepare Correctly for Accurate Results
Preparation for a fasting sugar test is simple in concept but important in detail. Most laboratories recommend fasting for 8 to 12 hours before the blood draw, with water allowed. Black coffee or unsweetened tea may or may not be permitted depending on the lab and clinician preference, but because caffeine can influence stress hormones and glucose in some people, water-only fasting is often the cleanest approach. Alcohol the night before can disrupt liver metabolism and sleep, potentially altering fasting glucose, so avoiding alcohol for at least 24 hours prior is a sensible precaution. Heavy exercise late in the evening can also affect glucose dynamics, sometimes lowering glucose through increased muscle uptake or, in some cases, raising it via stress hormones if the workout is intense. Keeping the day before the test relatively typical—without unusual dietary restriction or extreme exercise—often yields the most representative baseline.
Medication instructions should be clarified in advance. Some medications must be taken as usual, while others may be timed differently on the morning of the test. For people using insulin or glucose-lowering drugs, fasting can increase the risk of low blood sugar, so individualized guidance is essential. Sleep matters too: short or fragmented sleep can elevate morning glucose, and a late night can shorten or lengthen the fasting window unintentionally. Hydration also plays a role; dehydration can concentrate blood components and may slightly skew measurements. The goal is not to “game” the result but to capture a realistic fasting baseline. If you are ill, under acute stress, or recovering from surgery, it may be better to postpone unless the test is urgent, because illness-related hormone changes can temporarily raise glucose and make interpretation difficult. If you’re looking for fasting sugar test, this is your best choice.
What the Numbers Mean: Typical Ranges and Interpretation
Interpreting fasting glucose values depends on the measurement unit and the reference ranges used by the laboratory, but common cutoffs are widely recognized. In many settings, a fasting glucose below about 100 mg/dL (5.6 mmol/L) is considered normal. Values from about 100 to 125 mg/dL (5.6 to 6.9 mmol/L) are often categorized as impaired fasting glucose, commonly associated with prediabetes. A fasting result of 126 mg/dL (7.0 mmol/L) or higher on more than one occasion is frequently used as a diagnostic threshold for diabetes. These cutoffs are not arbitrary; they correlate with increasing risk of long-term complications, though risk exists on a continuum. That is why clinicians often consider the whole clinical picture—blood pressure, lipid profile, waist circumference, family history, and lifestyle factors—rather than relying only on a single fasting value. If you’re looking for fasting sugar test, this is your best choice.
A single elevated fasting reading does not automatically confirm a diagnosis. Laboratory errors, recent illness, inadequate fasting, and stress can produce a temporary rise. Many providers will repeat the fasting blood sugar test on another day or confirm with A1C, which reflects average glucose over roughly three months. Some people have normal fasting glucose but elevated A1C, suggesting frequent post-meal spikes; others have higher fasting glucose with a relatively modest A1C, sometimes driven by the dawn phenomenon or increased hepatic glucose output. Understanding trends is critical. If your fasting glucose is near the upper end of normal, it can be a prompt to focus on sleep, activity, and nutrition before the value crosses into a higher risk category. If it’s already in the prediabetes range, early action can significantly reduce progression risk. If it’s in the diabetes range, the next steps typically include confirmatory testing, evaluation for symptoms, and a treatment plan that may include lifestyle changes and medication. If you’re looking for fasting sugar test, this is your best choice.
Fasting Sugar Test vs A1C vs Oral Glucose Tolerance
The fasting sugar test is often compared with A1C and the oral glucose tolerance test (OGTT), and each tool offers different insights. Fasting glucose measures a single time point and is most sensitive to hepatic glucose output and basal insulin function. A1C reflects glycation of hemoglobin and provides a longer-term average that is less affected by day-to-day fluctuations. However, A1C can be influenced by conditions affecting red blood cell turnover, such as anemia, recent blood loss, certain hemoglobin variants, kidney disease, or pregnancy. The OGTT measures how the body handles a standardized glucose load over time, typically assessing glucose at fasting and then at intervals after drinking a glucose solution. This can reveal post-challenge abnormalities that a fasting test might miss, making it useful for diagnosing impaired glucose tolerance and gestational diabetes screening protocols.
Choosing the right test depends on the context. For routine screening, a fasting glucose test can be convenient, accessible, and cost-effective. For people with borderline fasting results, symptoms suggestive of glucose spikes, or discordant A1C results, an OGTT may provide clarity. For ongoing monitoring, A1C is commonly used because it reflects longer-term control, but fasting readings can still be helpful for day-to-day management, especially for people using home glucose meters or continuous glucose monitors. Some clinicians use a combination: fasting glucose for baseline, A1C for trend, and targeted post-meal checks to understand dietary response. Rather than viewing these tests as competitors, it is more useful to see them as complementary measurements that, together, describe fasting regulation, average exposure, and dynamic response to glucose intake. If you’re looking for fasting sugar test, this is your best choice.
Factors That Can Skew a Fasting Sugar Test Result
Many variables can influence a fasting sugar test, sometimes pushing the result higher or lower than expected. Acute illness is a major one: infections and inflammation increase stress hormones that raise blood glucose to supply immune function and tissue repair. Even a cold, dental infection, or flare of chronic inflammation can elevate fasting readings. Psychological stress can have a similar effect through cortisol and adrenaline, and that effect may be more pronounced in people already experiencing insulin resistance. Sleep loss is another common disruptor; a few nights of poor sleep can impair insulin sensitivity and increase morning glucose. Shift work and irregular sleep schedules can compound this by disrupting circadian rhythms, which are closely linked to glucose metabolism.
Expert Insight
Schedule your fasting sugar test for the morning and fast for 8–12 hours beforehand; drink only water and avoid alcohol and unusually heavy exercise the day prior. Take medications as directed by your clinician, and if you’re unsure whether to pause anything (especially diabetes medicines), confirm instructions before the test.
Keep results reliable by controlling the details: note your fasting duration, sleep quality, and any illness or stress, then share these with your healthcare provider. If a result is borderline or unexpected, repeat the test under the same conditions or ask about confirmatory options like an A1C or oral glucose tolerance test. If you’re looking for fasting sugar test, this is your best choice.
Diet and activity patterns in the days leading up to the test also matter. Extremely low carbohydrate intake can lower average glucose for some people, but it can also raise fasting glucose in others due to adaptive increases in hepatic glucose output, especially if the body is under stress. Conversely, very high carbohydrate intake the night before can lead to higher morning glucose if insulin response is sluggish. Intense exercise can temporarily increase glucose via stress hormones, while moderate activity often improves insulin sensitivity and may lower fasting levels. Medications are another key influence: corticosteroids, some diuretics, and certain psychiatric medications can raise glucose, while insulin and other glucose-lowering drugs can reduce it. Dehydration, smoking, and even pain can affect results. If a result seems inconsistent with your typical readings or symptoms, repeating the fasting blood sugar test under stable conditions is often the best way to confirm whether the number reflects a real metabolic pattern. If you’re looking for fasting sugar test, this is your best choice.
What to Expect During the Test and Afterward
A fasting sugar test is typically performed as a venous blood draw in a clinic or laboratory, though some settings may use a capillary fingerstick for quick screening. Venous testing is generally considered more accurate and standardized. After confirming your fasting status and basic information, a phlebotomist draws a small tube of blood, which is then analyzed for plasma glucose. The process usually takes only a few minutes. Some people feel lightheaded during blood draws, especially when fasting, so it can help to sit or lie down if you have a history of fainting. Drinking water beforehand is usually allowed and can make veins easier to access. After the draw, you can typically eat and drink normally unless other tests are being performed that require continued fasting.
| Test type | When it’s taken | What it indicates |
|---|---|---|
| Fasting blood sugar (FBS) | After 8–12 hours of fasting (usually morning) | Baseline blood glucose level; helps screen for prediabetes/diabetes |
| Random blood sugar (RBS) | Any time of day, with no fasting required | Current glucose at that moment; useful for quick checks and symptom evaluation |
| HbA1c (A1C) | Any time; no fasting needed | Average blood sugar over ~2–3 months; helps diagnose and monitor diabetes control |
Results may be available the same day or within a couple of days, depending on the lab. It’s useful to review the value alongside previous results, if available, rather than treating it as a standalone score. If the fasting glucose test is normal but risk factors are present, clinicians may recommend periodic retesting, often annually or every few years depending on the situation. If the result is elevated, the next steps might include repeat testing, an A1C, or additional metabolic labs such as fasting insulin, lipid panel, or liver enzymes. Some providers may also recommend home monitoring to understand patterns, especially if symptoms suggest swings between high and low glucose. If you feel shaky, sweaty, confused, or unusually weak after fasting—particularly if you take glucose-lowering medication—eating promptly and contacting your clinician is important. For most people, however, the test is routine and straightforward, and the value lies in using the information to guide practical, sustainable health decisions. If you’re looking for fasting sugar test, this is your best choice.
Improving Fasting Glucose Through Lifestyle Changes
If a fasting sugar test indicates impaired fasting glucose or trends upward over time, lifestyle changes can be highly effective. Regular physical activity improves insulin sensitivity by increasing glucose uptake into muscle cells and enhancing mitochondrial function. Both aerobic exercise (like brisk walking, cycling, or swimming) and resistance training (like weights or bodyweight exercises) can lower fasting glucose, and combining them often produces the strongest effect. Consistency matters more than intensity for most people. Even short bouts of movement after meals can reduce overall glucose exposure and may improve fasting values over weeks to months. For people who sit for long periods, breaking up sedentary time with brief walks can meaningfully improve metabolic markers.
Nutrition strategies often focus on reducing refined carbohydrates and added sugars while increasing fiber, protein, and healthy fats to improve satiety and blunt glucose spikes. Prioritizing minimally processed foods—vegetables, legumes, whole grains in appropriate portions, nuts, seeds, lean proteins, and unsweetened dairy or alternatives—can support better glucose regulation. Timing can also matter: late-night large meals may worsen morning readings in some individuals, while a balanced dinner eaten earlier can improve fasting results. Sleep and stress management are frequently overlooked yet powerful. Improving sleep duration and quality can reduce insulin resistance, and stress reduction practices—such as regular relaxation routines, breathing exercises, or counseling—can lower stress hormone-driven glucose elevation. Weight loss, when appropriate, often improves fasting glucose by reducing liver fat and visceral fat. Even a modest reduction in body weight can shift fasting blood sugar toward a healthier range. The key is choosing changes that are realistic enough to maintain long-term, because fasting levels reflect ongoing physiology rather than a short-term fix. If you’re looking for fasting sugar test, this is your best choice.
Medical Next Steps When Results Are High
When a fasting sugar test is repeatedly high, medical evaluation becomes important to confirm the diagnosis and identify the best treatment approach. A clinician may repeat the fasting glucose test, order an A1C, or recommend an oral glucose tolerance test to clarify whether the pattern is prediabetes or diabetes. They may also look for contributing conditions such as thyroid disorders, Cushing’s syndrome, sleep apnea, or medication-related hyperglycemia. Additional labs may include kidney function tests, urine albumin, lipid profile, and liver enzymes, because glucose dysregulation often travels with cardiovascular and liver risks. Blood pressure and waist circumference may be assessed as part of a broader metabolic evaluation. This bigger picture helps determine how aggressive management should be and which risk factors deserve immediate attention.
Treatment can range from structured lifestyle therapy to medication. In prediabetes, some people benefit from targeted weight management, increased activity, and dietary changes alone, while others—especially with higher risk—may be offered medications such as metformin. In type 2 diabetes, medication choices depend on individual factors: baseline A1C, body weight goals, heart and kidney health, cost considerations, and side effect profiles. Some medications reduce liver glucose output, others increase insulin sensitivity, and others affect appetite or glucose excretion through the kidneys. For people with very high fasting levels or symptoms, insulin may be needed initially. Monitoring plans can include periodic lab testing and, for some, home glucose monitoring to understand fasting patterns and responses to meals. The goal is not only to lower the fasting number but also to reduce overall glucose exposure and protect organs over time. Prompt follow-up after an abnormal fasting blood sugar test is important because early management can prevent progression and reduce complication risk substantially. If you’re looking for fasting sugar test, this is your best choice.
Using Home Monitoring to Complement a Fasting Sugar Test
Home monitoring can provide context that a single fasting sugar test cannot. A lab fasting glucose value is a snapshot, while a home glucometer or continuous glucose monitor (CGM) can reveal daily patterns, including how sleep, stress, and dinner timing affect morning readings. For someone with borderline fasting results, checking fasting glucose at home for several mornings—under consistent conditions—can help determine whether the lab value reflects a typical baseline or an outlier. Home readings are not always identical to lab measurements due to device variability, but patterns over time can still be highly informative. Many people find it helpful to record sleep duration, exercise, evening meal composition, and alcohol intake alongside morning glucose to identify triggers of higher fasting values.
Post-meal checks can also be useful. Some people have normal fasting glucose but significant postprandial spikes, which can still contribute to elevated A1C and long-term risk. Measuring glucose one to two hours after meals, under clinician guidance, can highlight which foods or portion sizes lead to higher peaks. This information can support practical adjustments like adding fiber, increasing protein, choosing lower-glycemic carbohydrates, or taking a walk after eating. For people already diagnosed with diabetes, home monitoring supports medication adjustments and helps prevent hypoglycemia. However, it’s important not to become overly reactive to single readings; glucose naturally fluctuates. The value lies in trends and in learning how behaviors influence the numbers. When combined with periodic lab work, home monitoring can turn the fasting sugar test from a one-time event into part of a coherent feedback system for metabolic health.
Common Mistakes to Avoid Before and After Testing
Several avoidable mistakes can reduce the usefulness of a fasting sugar test. One of the most common is not following the fasting window correctly. Eating late at night, adding sugar or cream to coffee, or drinking caloric beverages in the morning can raise glucose and invalidate the “fasting” condition. Another mistake is extending the fast too long in an attempt to get a “better” number. Prolonged fasting can alter hormone levels and, in some people, increase glucose through counter-regulatory responses. Overexercising right before the test can also distort results, either by raising glucose through stress hormones or by lowering it through increased muscle uptake. Keeping the day before the test routine and the morning calm tends to provide the most reliable baseline measurement.
After testing, a frequent mistake is overinterpreting a single result without considering context. A mildly elevated fasting glucose may be temporary due to poor sleep, stress, or a recent illness. Conversely, a normal result does not automatically mean there is no risk, especially if there are strong risk factors or symptoms. Another pitfall is making drastic dietary changes based solely on one reading, such as severely restricting food groups, which can be difficult to sustain and may backfire. A better approach is to confirm abnormal results and then implement measured changes that can be maintained. It’s also important to avoid delaying follow-up when fasting glucose is in the diabetes range, because early treatment can protect the eyes, kidneys, nerves, and cardiovascular system. Using the fasting blood sugar test as one data point—paired with repeat testing, A1C, and lifestyle assessment—helps ensure decisions are grounded in a reliable understanding of your metabolic health. If you’re looking for fasting sugar test, this is your best choice.
Long-Term Tracking and What a Healthy Trend Looks Like
Long-term tracking turns the fasting sugar test into a meaningful indicator rather than a periodic surprise. A single value can be influenced by random factors, but a series of fasting glucose results over months or years can reveal whether your baseline glucose regulation is stable, improving, or worsening. A healthy trend is typically one where fasting glucose remains in the normal range with minimal upward drift over time, especially as life circumstances change. If values are in the prediabetes range, a healthy trend might be gradual reduction toward normal, or at least stability without progression. Because glucose regulation can change with age, weight gain, changes in activity, new medications, or sleep disruption, periodic monitoring can catch issues early when they are most reversible. Keeping results in a personal health record, along with notes about major lifestyle changes, can help you and your clinician interpret shifts more accurately.
It’s also useful to define success beyond a single fasting number. Improvements in waist circumference, blood pressure, triglycerides, HDL cholesterol, liver enzymes, and energy levels often move together with better glucose control. If fasting glucose improves but other risk markers worsen, the overall plan may need adjustment. If fasting glucose remains stubbornly elevated despite lifestyle changes, that can be a signal to evaluate sleep apnea, chronic stress, medication effects, or underlying endocrine issues, and to consider medical therapy sooner rather than later. For many people, the most sustainable progress comes from small, repeatable actions: consistent movement, higher-fiber meals, adequate protein, better sleep routines, and reduced intake of sugary drinks and refined snacks. When these habits are in place, the fasting sugar test often becomes a reassuring confirmation that the body’s baseline glucose regulation is moving in a healthier direction, and that progress is being maintained over time.
Watch the demonstration video
In this video, you’ll learn what a fasting blood sugar test measures, how to prepare for it, and why fasting matters for accurate results. It explains when the test is recommended, what your numbers may indicate about blood sugar control, and what to do next if your results are high or low. If you’re looking for fasting sugar test, this is your best choice.
Summary
In summary, “fasting sugar test” is a crucial topic that deserves thoughtful consideration. We hope this article has provided you with a comprehensive understanding to help you make better decisions.
Frequently Asked Questions
What is a fasting sugar test?
A **fasting sugar test** is a simple blood test that checks your blood glucose level after you’ve gone without eating for a certain number of hours. It’s commonly used to screen for diabetes and to help monitor how well blood sugar is being managed over time.
How long should I fast before a fasting sugar test?
Typically 8–12 hours. Water is usually allowed, but follow your lab or clinician’s instructions.
Can I drink water, coffee, or tea while fasting?
Plain water is usually fine to drink beforehand. However, steer clear of coffee or tea—even black—unless your clinician specifically approves, since these drinks can influence some people’s results on a **fasting sugar test**.
Should I take my usual medications before the test?
Check with your clinician first. Some medications—such as diabetes drugs, steroids, and certain diuretics—can shift your glucose levels, so you may need to adjust the timing or dose before your **fasting sugar test**.
What is a normal fasting blood sugar result?
Common reference ranges: normal <100 mg/dL (5.6 mmol/L); prediabetes 100–125 mg/dL (5.6–6.9); diabetes ≥126 mg/dL (≥7.0) on repeat testing.
What can affect fasting sugar test results?
Illness, stress, and poor sleep can all throw off your **fasting sugar test** results, and so can recent alcohol use, intense exercise, or certain medications. Even small slip-ups—like not truly fasting—may raise or lower your reading.
📢 Looking for more info about fasting sugar test? Follow Our Site for updates and tips!
Trusted External Sources
- Fasting Blood Sugar: Testing, Levels & What They Mean
On Jan 31, 2026, a **fasting sugar test** checks the amount of glucose in your blood after you haven’t eaten for a set period of time. It’s a quick, widely used screening tool to help spot **prediabetes**, **diabetes**, or **gestational diabetes** early.
- Diabetes Testing – CDC
On May 15, 2026, your doctor may recommend an A1C test—often alongside a **fasting sugar test**—to get a clearer picture of your blood glucose. The A1C measures your average blood sugar over the past two to three months: **below 5.7%** is considered normal, **5.7%–6.4%** suggests prediabetes, and **6.5% or higher** typically indicates diabetes.
- Diabetes – Diagnosis and treatment – Mayo Clinic
On Jan 21, 2026, a glucose tolerance test may be used to see how your body handles sugar. You’ll fast overnight, then your healthcare provider will take an initial blood sample—often called a **fasting sugar test**—to measure your baseline blood glucose. After that, you’ll drink a sweet liquid, and your blood sugar will be checked again at set intervals to track how it changes over time.
- Blood sugar test – UCSF Health
As of Feb 10, 2026, a typical **fasting sugar test** (also called a fasting blood glucose test) is considered normal when your blood glucose falls between **70 and 99 mg/dL** (**3.9 to 5.5 mmol/L**).
- Blood Glucose Monitoring – StatPearls – NCBI Bookshelf – NIH
As of Apr 23, 2026, routine blood glucose monitoring is typically done before meals and at bedtime for clients who are able to eat. For those receiving enteral nutrition or who are nil by oris (NPO), schedules may be adjusted—often starting with a **fasting sugar test** and then continuing at intervals that match their feeding plan and clinical needs.