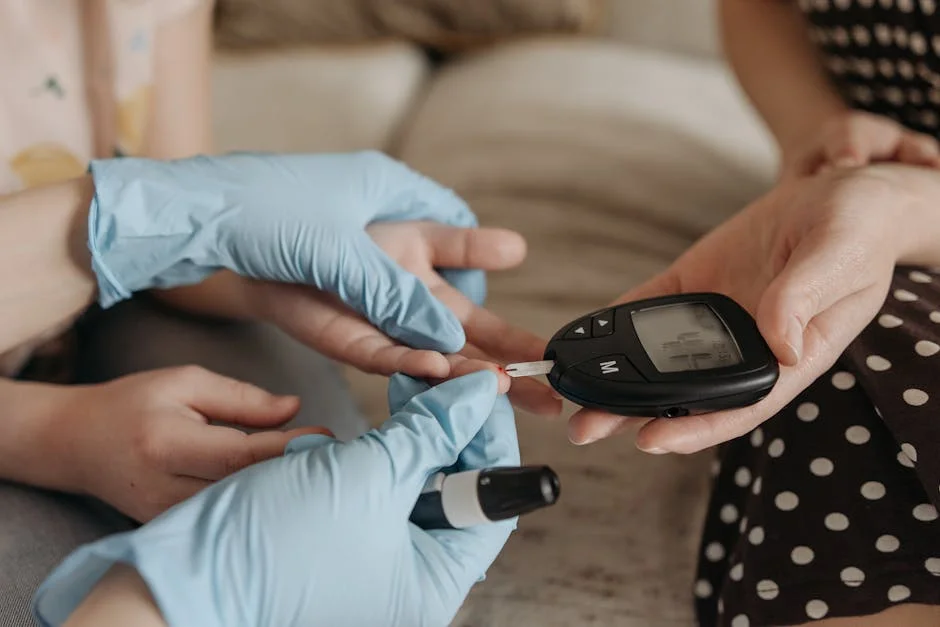
The glucose fasting test is a common blood test that measures how much glucose (sugar) is circulating in your bloodstream after you have not eaten for a set period, usually 8 to 12 hours. Because food directly affects blood sugar, fasting creates a more standardized baseline so the result reflects how your body regulates glucose when it is not actively processing a meal. Clinicians use fasting glucose results to screen for diabetes, identify prediabetes, evaluate unexplained symptoms such as increased thirst or frequent urination, and monitor how well lifestyle changes or medications are working. While a single number cannot capture every aspect of metabolic health, fasting glucose is a foundational data point that often triggers further testing or follow-up. It is also relatively simple to perform, widely available, and inexpensive compared with more specialized evaluations, which is why it is frequently ordered during annual checkups or routine lab panels.
Table of Contents
- My Personal Experience
- Understanding the glucose fasting test and why it matters
- How fasting blood glucose reflects metabolism and insulin function
- Who should consider a glucose fasting test and how often it is ordered
- How to prepare for a glucose fasting test for accurate results
- What happens during the test and what the lab actually measures
- Interpreting results: normal, prediabetes, and diabetes ranges
- Factors that can falsely raise or lower fasting glucose
- Glucose fasting test compared with A1C and oral glucose tolerance testing
- Expert Insight
- What elevated fasting glucose can mean for long-term health
- Steps that may help improve fasting glucose (lifestyle and clinical options)
- Special considerations: pregnancy, older adults, and people on glucose-lowering medication
- Getting the most from your results: follow-up, repeat testing, and tracking trends
- Practical tips for the day before and the morning of your blood draw
- Conclusion: using the glucose fasting test as a tool for prevention and better health
- Watch the demonstration video
- Frequently Asked Questions
- Trusted External Sources
My Personal Experience
I had to do a fasting glucose test after my annual physical showed my blood sugar was a little high. The night before, I stopped eating after dinner and kept double-checking the time because I didn’t want to mess it up. By morning I was surprisingly cranky and had a mild headache, and sitting in the waiting room while other people sipped coffee felt like torture. The blood draw itself was quick—just a pinch—and the nurse reminded me to eat something right after, which I did in the parking lot with a granola bar I’d brought along. Waiting for the results was the worst part, but when my doctor called, she said it was borderline and suggested I tighten up my diet and recheck in a few months. It wasn’t dramatic, but it definitely made me pay more attention to what I eat and how often I’m moving during the day. If you’re looking for glucose fasting test, this is your best choice.
Understanding the glucose fasting test and why it matters
The glucose fasting test is a common blood test that measures how much glucose (sugar) is circulating in your bloodstream after you have not eaten for a set period, usually 8 to 12 hours. Because food directly affects blood sugar, fasting creates a more standardized baseline so the result reflects how your body regulates glucose when it is not actively processing a meal. Clinicians use fasting glucose results to screen for diabetes, identify prediabetes, evaluate unexplained symptoms such as increased thirst or frequent urination, and monitor how well lifestyle changes or medications are working. While a single number cannot capture every aspect of metabolic health, fasting glucose is a foundational data point that often triggers further testing or follow-up. It is also relatively simple to perform, widely available, and inexpensive compared with more specialized evaluations, which is why it is frequently ordered during annual checkups or routine lab panels.
Even though the glucose fasting test is straightforward, the implications of the results can be significant. Blood sugar regulation depends on a complex interplay of insulin production in the pancreas, insulin sensitivity in muscle and fat tissue, liver glucose output, sleep and stress hormones, physical activity, and even certain medications. A fasting result that is higher than expected may indicate insulin resistance, impaired glucose regulation, undiagnosed diabetes, or temporary elevations related to acute illness, poor sleep, or stress. Conversely, an unusually low result could point to medication effects, prolonged fasting, endocrine issues, or other health concerns that require evaluation. Understanding what the test measures, how to prepare, and what can influence the numbers helps you interpret results more confidently and communicate effectively with your healthcare provider. Accurate preparation and context are essential so decisions are based on meaningful data rather than a misleading snapshot.
How fasting blood glucose reflects metabolism and insulin function
Fasting blood glucose is often described as a window into baseline metabolism because it captures the balance between glucose entering the bloodstream and glucose being removed from it when you have not eaten. During fasting, most glucose comes from the liver, which releases glucose through glycogen breakdown and gluconeogenesis. Insulin, even at low fasting levels, acts like a brake on liver glucose output and helps tissues take up glucose. When insulin sensitivity is strong, the liver does not release excessive glucose, and muscles and other tissues respond efficiently, keeping fasting levels in a healthy range. When insulin resistance develops, the liver may continue producing glucose despite insulin signals, and tissues may not take up glucose as readily. The result can be a gradual rise in fasting glucose over time, sometimes years before diabetes is diagnosed. This is why the glucose fasting test is used as an early screening tool: it can reveal changes before symptoms become obvious.
That said, fasting glucose is only one piece of the metabolic picture. Some people maintain near-normal fasting levels yet experience high blood sugar after meals, while others show elevated fasting values with only modest post-meal spikes. Differences can relate to the timing and pattern of insulin secretion, the liver’s glucose production, muscle mass, physical activity, and genetics. Sleep deprivation and chronic stress may also raise morning glucose by increasing cortisol and other counter-regulatory hormones that signal the liver to release more sugar. Certain medications, including some steroids and antipsychotics, can raise blood glucose as well. Because of these variables, clinicians may pair the glucose fasting test with A1C, oral glucose tolerance testing, or home glucose monitoring, depending on your risk factors and symptoms. A fasting number is informative, but its greatest value comes from interpreting it in context and, when needed, confirming patterns over time.
Who should consider a glucose fasting test and how often it is ordered
Many adults receive a glucose fasting test as part of routine preventive care, especially if they have risk factors for diabetes. Common risk factors include being overweight, having a sedentary lifestyle, a family history of type 2 diabetes, a history of gestational diabetes, polycystic ovary syndrome (PCOS), high blood pressure, abnormal cholesterol or triglycerides, or belonging to an ethnic group with higher diabetes prevalence. Age is also a factor, as insulin sensitivity can decline over time. Clinicians may recommend fasting glucose screening more frequently when risk is higher or when prior results were borderline. For someone with no major risk factors and previously normal results, testing may be less frequent, often aligned with annual or periodic wellness labs. For those with prediabetes, repeat testing might occur every 3 to 12 months to track trends and assess whether interventions are working.
There are also symptom-driven reasons to order a fasting glucose test. Persistent thirst, frequent urination, unexplained weight loss, blurry vision, fatigue, slow wound healing, frequent infections, or tingling in hands and feet can all be associated with elevated blood sugar. On the other end of the spectrum, episodes of shakiness, sweating, confusion, or dizziness—especially if related to fasting or medication use—may prompt evaluation for low blood sugar. Pregnancy is a special situation: while the glucose fasting test can be part of early pregnancy screening in some cases, gestational diabetes is often assessed with specific glucose challenge or tolerance protocols. People already diagnosed with diabetes may still have fasting glucose measured in labs, but daily management often relies more on home testing, continuous glucose monitors, and A1C. The decision about who needs testing, and how often, is best personalized, balancing risk, prior results, and any changes in health status.
How to prepare for a glucose fasting test for accurate results
Preparation is critical because small deviations can meaningfully change fasting glucose values. Most laboratories and clinicians instruct you to fast for 8 to 12 hours before the blood draw. “Fasting” generally means no food and no caloric beverages, including coffee with cream or sugar, juice, soda, and alcohol. Plain water is typically allowed and encouraged because dehydration can make blood draws harder and may slightly affect lab values. If your appointment is in the morning, an overnight fast is often easiest: finish dinner, avoid late-night snacks, and have the test done early. If the test is scheduled later in the day, follow the lab’s guidance carefully and plan your fasting window so it does not become excessively long, which can sometimes lower glucose in some people or trigger stress hormone responses in others. Aim for consistency: if repeat testing is planned, try to fast for a similar duration each time. If you’re looking for glucose fasting test, this is your best choice.
Medication guidance is equally important. Some medications can raise or lower blood sugar, and others should not be skipped. If you take insulin or glucose-lowering medications, ask your clinician whether to adjust the dose the night before or the morning of the test to reduce the risk of hypoglycemia. Never stop prescribed medications without explicit instructions. If you take steroids, certain diuretics, beta-blockers, or antipsychotics, disclose them because they may influence glucose and interpretation. Also consider lifestyle factors the day before: intense exercise can lower glucose for some people and raise it for others through stress hormones, so it’s wise to keep activity moderate and typical. Poor sleep and acute stress can elevate morning glucose, so do what you can to rest. Avoid heavy alcohol intake the night before because it can disrupt glucose regulation and liver metabolism. When you arrive, inform the phlebotomist and clinician of your fasting duration, recent illness, and any unusual circumstances so results can be interpreted appropriately. If you’re looking for glucose fasting test, this is your best choice.
What happens during the test and what the lab actually measures
The glucose fasting test usually involves a standard venous blood draw from a vein in your arm. The sample is then analyzed for plasma glucose concentration, typically reported in milligrams per deciliter (mg/dL) in the United States or millimoles per liter (mmol/L) in many other countries. The measurement reflects glucose dissolved in the plasma portion of blood. Laboratories use specific analytic methods to quantify glucose, and results are generally reliable when proper handling occurs. Because glucose can be consumed by blood cells after the draw, labs follow protocols to process samples promptly or use tubes with preservatives that stabilize glucose levels. That is one reason it is helpful to use a reputable lab and to have repeat tests performed under similar conditions when monitoring trends.
Some people confuse fasting plasma glucose with fingerstick readings from a home glucometer. Home meters are useful for day-to-day monitoring, but they can have wider variability and are influenced by technique, strip quality, and whether the reading is capillary blood rather than venous plasma. The lab-based glucose fasting test is considered the standard for diagnosis and screening. In some settings, a clinician may also order related tests at the same time, such as A1C, lipid panel, kidney function, liver enzymes, or insulin levels, depending on the clinical question. You may also encounter a “basic metabolic panel” or “comprehensive metabolic panel,” which includes glucose but may not specify fasting unless instructed. If your goal is accurate fasting glucose assessment, confirm that the ordering provider and lab are expecting a fasting sample. Clear labeling and communication reduce confusion and help ensure the result answers the intended question.
Interpreting results: normal, prediabetes, and diabetes ranges
Interpreting a glucose fasting test involves comparing your number to established clinical thresholds and considering your overall health context. Commonly used categories for fasting plasma glucose are: normal (typically below 100 mg/dL or below 5.6 mmol/L), impaired fasting glucose/prediabetes (often 100–125 mg/dL or 5.6–6.9 mmol/L), and diabetes (usually 126 mg/dL or 7.0 mmol/L and above) when confirmed on a repeat test or supported by other diagnostic criteria. These thresholds may vary slightly based on local guidelines, lab reporting, and clinical judgment, but they provide a practical framework. If your result falls in the prediabetes range, it suggests that glucose regulation is impaired and that the risk of progressing to type 2 diabetes is higher, especially without lifestyle changes. Many people in this range have no symptoms, which is why screening is valuable.
A single elevated fasting glucose does not always equal a definitive diagnosis. Illness, stress, sleep deprivation, recent steroid use, and other temporary factors can push glucose higher. For that reason, clinicians often repeat the glucose fasting test on a different day or use another diagnostic method such as A1C or an oral glucose tolerance test. If results are borderline, your provider may look for consistency across multiple measurements or consider additional markers of cardiometabolic risk, such as blood pressure, triglycerides, HDL cholesterol, waist circumference, and family history. If your fasting glucose is normal but you have strong risk factors or symptoms, further testing may still be appropriate because some people have normal fasting values but elevated post-meal glucose. The key is to treat the number as a signal that guides next steps rather than a verdict in isolation.
Factors that can falsely raise or lower fasting glucose
Many everyday factors can influence fasting glucose and potentially lead to results that are higher or lower than your typical baseline. Acute illness is a major one: infections, inflammation, and fever can increase stress hormones such as cortisol and adrenaline, prompting the liver to release more glucose. Sleep loss has a similar effect, and even a single short night can reduce insulin sensitivity temporarily. Psychological stress, pain, and anxiety about the blood draw can also raise glucose in some individuals. Timing matters too: the “dawn phenomenon,” a natural early-morning rise in blood sugar driven by hormones, can make morning fasting readings higher for some people, especially those with insulin resistance or diabetes. Longer-than-recommended fasting can complicate interpretation: while some people may see lower glucose after prolonged fasting, others may see higher numbers due to counter-regulatory hormone release and increased liver glucose output. If you’re looking for glucose fasting test, this is your best choice.
On the other side, fasting glucose can be artificially low due to certain medications (including insulin, sulfonylureas, and other glucose-lowering drugs), heavy alcohol use, prolonged fasting beyond the intended window, or rare endocrine disorders. Intense exercise the day before can lower glucose by increasing muscle glucose uptake and improving insulin sensitivity, but very strenuous activity can also transiently raise glucose due to stress hormone release, especially if combined with inadequate sleep or under-fueling. Laboratory and pre-analytic factors can matter as well: delays in processing the sample may lower measured glucose if preservatives are not used, and differences between plasma and whole blood measurements can cause confusion when comparing lab values to home readings. Because so many variables can affect a glucose fasting test, it helps to document anything unusual—recent illness, medication changes, atypical exercise, poor sleep, or alcohol intake—so your clinician can decide whether the result reflects your usual physiology or a temporary distortion.
Glucose fasting test compared with A1C and oral glucose tolerance testing
The glucose fasting test is often paired with other methods because each test captures a different aspect of glucose regulation. Fasting plasma glucose reflects a single moment under standardized conditions, mainly influenced by liver glucose output and baseline insulin activity. Hemoglobin A1C, by contrast, estimates average blood sugar over roughly the past 2 to 3 months by measuring the percentage of hemoglobin molecules in red blood cells that have glucose attached. A1C can be convenient because it does not require fasting, and it provides a broader view than a single fasting measurement. However, A1C can be less reliable in certain situations, such as anemia, recent blood loss, hemoglobin variants, kidney disease, or conditions that alter red blood cell lifespan. In those cases, the glucose fasting test may be more dependable, or clinicians may use alternative markers like fructosamine.
| Aspect | Glucose Fasting Test | HbA1c Test | Oral Glucose Tolerance Test (OGTT) |
|---|---|---|---|
| What it measures | Blood glucose level after an overnight fast (typically 8–12 hours) | Average blood glucose over the past ~2–3 months | Body’s response to a glucose drink, measured over time (often 2 hours) |
| When it’s used | Screening/diagnosis of prediabetes and diabetes; monitoring fasting glucose trends | Screening/diagnosis and long-term monitoring of diabetes control | Clarifying borderline results; diagnosing gestational diabetes and impaired glucose tolerance |
| Key considerations | Requires fasting; can be affected by acute illness, stress, or certain medications | No fasting needed; may be less accurate with some anemias/hemoglobin variants | More time-consuming; requires fasting and multiple blood draws; can cause nausea |
Expert Insight
Schedule your glucose fasting test for the morning and fast for 8–12 hours beforehand (water is fine). Avoid alcohol and unusually intense exercise the day before, and ask your clinician whether to take morning medications as usual—some drugs can affect results.
On test day, keep your routine steady: drink water, skip coffee and gum, and don’t smoke before the blood draw. Afterward, eat a balanced meal with protein and fiber, and request a copy of your results so you can track trends over time and discuss next steps if values are borderline. If you’re looking for glucose fasting test, this is your best choice.
The oral glucose tolerance test (OGTT) evaluates how your body handles a standardized glucose load over time, typically measuring glucose at fasting and again at set intervals after drinking a glucose solution. This approach can uncover impaired glucose tolerance that may not show up on fasting labs, making it useful for diagnosing gestational diabetes and for clarifying borderline or conflicting results. The OGTT is more time-consuming and can be less convenient, but it provides dynamic information about post-meal glucose handling and insulin response. In practice, clinicians choose among these tests based on your risk profile, symptoms, pregnancy status, and how clear the diagnosis is from initial screening. Many people start with a glucose fasting test because it is accessible and easy to standardize, then move to A1C or OGTT if additional detail is needed.
What elevated fasting glucose can mean for long-term health
Persistently elevated fasting glucose, even in the prediabetes range, can signal underlying insulin resistance and increased cardiometabolic risk. Over time, higher blood sugar can contribute to inflammation, oxidative stress, and damage to blood vessels, which may raise the risk of heart disease and stroke. Prediabetes is also associated with fatty liver disease, hypertension, abnormal cholesterol patterns (often higher triglycerides and lower HDL), and increased abdominal fat. While not everyone with elevated fasting glucose progresses to type 2 diabetes, the risk is meaningful, especially when combined with other factors like family history, inactivity, or weight gain. The value of detecting elevated fasting glucose early is that it creates an opportunity to intervene before complications develop. Improvements in diet quality, physical activity, sleep, stress management, and weight reduction—when appropriate—can substantially reduce diabetes risk and may return fasting glucose to a healthier range. If you’re looking for glucose fasting test, this is your best choice.
If fasting glucose is in the diabetes range, the health implications depend on how long blood sugar has been elevated and whether other risk factors are present. Chronically high glucose can affect small blood vessels in the eyes, kidneys, and nerves, and it can also accelerate atherosclerosis in larger arteries. However, outcomes vary widely, and many people achieve excellent health with timely diagnosis, consistent management, and regular monitoring. The glucose fasting test can also be used as a follow-up tool: trends over months can show whether lifestyle changes or medications are improving baseline glucose control. It is important to avoid self-diagnosis or panic based on a single reading; instead, use the result as a prompt to seek professional evaluation, confirm the finding, and create a plan. Early action tends to be more effective and less intensive than trying to reverse more advanced metabolic disease later.
Steps that may help improve fasting glucose (lifestyle and clinical options)
When a glucose fasting test suggests elevated baseline blood sugar, the most impactful steps often involve improving insulin sensitivity and reducing excess liver glucose output. Nutrition changes frequently start with reducing highly refined carbohydrates and added sugars, increasing fiber from vegetables, legumes, and whole grains as tolerated, and ensuring adequate protein to support satiety and muscle maintenance. Many people benefit from balancing carbohydrate intake across the day and pairing carbs with protein and healthy fats to blunt glucose spikes. Alcohol moderation can also help because alcohol can disrupt liver metabolism and sleep quality, both of which influence fasting glucose. Physical activity is another cornerstone: a mix of aerobic exercise and resistance training improves insulin sensitivity, increases muscle glucose uptake, and supports healthy body composition. Even consistent walking after meals can improve overall glycemic patterns, which may translate into better fasting numbers over time.
Sleep and stress deserve equal attention because cortisol and other stress hormones can elevate fasting glucose. A consistent sleep schedule, addressing sleep apnea if present, and practicing stress-reduction techniques can make a measurable difference for some people. Weight reduction, when medically appropriate, can significantly improve insulin resistance; even modest weight loss may lower fasting glucose. For some individuals, lifestyle measures are not enough or are difficult to sustain due to genetics, other medical conditions, or long-standing insulin resistance. In those cases, clinicians may recommend medications such as metformin for prediabetes or diabetes, and they may consider additional therapies if diabetes is diagnosed. The right plan depends on your overall risk, preferences, and any coexisting conditions. Importantly, any changes should be made with an emphasis on sustainability: dramatic short-term diets can lead to rebound effects, while gradual, consistent changes are more likely to improve fasting glucose and overall health long term. If you’re looking for glucose fasting test, this is your best choice.
Special considerations: pregnancy, older adults, and people on glucose-lowering medication
Pregnancy changes glucose metabolism due to hormonal shifts that increase insulin resistance as pregnancy progresses. While fasting glucose can be informative early in pregnancy, screening for gestational diabetes often relies on specific protocols such as a glucose challenge test and, if needed, an OGTT. A glucose fasting test may still be used in some settings to identify preexisting diabetes or early abnormalities, but interpretation should be done within pregnancy-specific guidance. Nutrition needs in pregnancy are unique, and any attempt to lower glucose should prioritize maternal and fetal health, adequate caloric intake, and appropriate weight gain as advised by a clinician. If fasting glucose is elevated during pregnancy, timely management is important because uncontrolled gestational diabetes can increase risks such as large birth weight, delivery complications, and future diabetes risk for both parent and child.
Older adults may have additional factors affecting fasting glucose interpretation, including changes in muscle mass, kidney function, medication burden, and risk of hypoglycemia. For an older person, the goal is often balanced: avoiding chronic high glucose while also preventing low blood sugar episodes that can cause falls or cognitive symptoms. People taking insulin or medications that increase insulin secretion need careful planning before a fasting lab. Skipping breakfast and taking the usual dose can lead to hypoglycemia, so clinicians often provide tailored instructions for the evening before and morning of the glucose fasting test. If you use a continuous glucose monitor, it can provide helpful context around the fasting period, but the lab value remains the diagnostic standard. Always report any low blood sugar symptoms during the fasting period to the clinical team, and bring a quick source of glucose for use immediately after the blood draw if needed.
Getting the most from your results: follow-up, repeat testing, and tracking trends
A glucose fasting test is most useful when it leads to clear next steps, whether that is reassurance, repeat testing, or a structured plan to reduce risk. If the result is normal, your clinician may still recommend periodic rescreening based on age and risk factors. If the result is borderline, repeating the test under consistent conditions is often recommended, sometimes along with an A1C to compare short-term baseline glucose with longer-term average glucose exposure. Tracking trends matters because small changes over time can be more informative than a single isolated number. If your fasting glucose has slowly increased across several tests, that pattern may indicate worsening insulin resistance even if you are not yet in the diabetes range. Conversely, improvements after lifestyle changes can validate that your efforts are working and can guide which habits to maintain.
Follow-up should also consider the broader cardiometabolic picture. Because insulin resistance often clusters with high blood pressure, abnormal lipids, and increased waist circumference, clinicians may evaluate these together rather than focusing solely on fasting glucose. If you are monitoring at home, discuss with your provider how home readings compare with lab results and whether additional checks, such as occasional post-meal readings, would be helpful. Keep in mind that lab glucose can vary day to day; hydration, sleep, stress, and recent activity can shift the number. To make your next glucose fasting test more comparable, aim for a similar fasting duration, avoid unusual late-night eating, keep alcohol moderate, and schedule the draw at a similar time of day. Most importantly, treat the result as actionable information, not a label: the goal is to use the data to reduce risk, improve energy and well-being, and prevent complications through consistent, evidence-based care.
Practical tips for the day before and the morning of your blood draw
The day before a glucose fasting test, aim for a normal routine rather than an extreme “pre-test” diet. Some people try to eat very little or avoid all carbohydrates in an attempt to influence the number, but this can make results less representative of your usual metabolism and may even backfire by increasing stress hormones or prompting unusual liver glucose output. A balanced dinner with fiber, protein, and a moderate amount of carbohydrates is often a sensible choice unless your clinician has given specific instructions. Hydrate with water throughout the day and evening, and avoid heavy alcohol intake. Try not to schedule intense workouts that are far outside your normal activity level, and prioritize sleep because poor sleep can raise morning glucose. If you are sick, especially with fever or significant infection, consider asking whether it is better to reschedule so the test reflects your typical baseline.
On the morning of the test, continue fasting as instructed and drink water if allowed. Avoid caloric beverages, including coffee with additives; if you normally drink black coffee, ask your lab or clinician whether it is permitted, as policies vary and caffeine may influence glucose in some individuals. Bring a snack for after the blood draw, especially if you are prone to feeling lightheaded or if you take medications that can lower blood sugar. If you have diabetes or prediabetes and monitor glucose at home, you may choose to check your level before leaving home for safety, particularly if you are fasting longer than usual. Arrive on time, inform staff of your fasting duration, and mention any medication changes, sleep disruption, or unusual stress. These details help interpret the glucose fasting test result accurately and determine whether any follow-up is needed.
Conclusion: using the glucose fasting test as a tool for prevention and better health
The glucose fasting test remains one of the most practical and widely used ways to assess baseline blood sugar control, offering a clear snapshot of how your body manages glucose when food is not influencing the result. When paired with good preparation and interpreted in context, it can identify early metabolic changes, guide decisions about additional testing, and motivate targeted lifestyle improvements that reduce long-term risk. If your number is higher than expected, it does not automatically define your future; it signals an opportunity to confirm the pattern, understand contributing factors like sleep, stress, medications, and activity, and take steps that improve insulin sensitivity and overall cardiometabolic health. With consistent follow-up and personalized care, the glucose fasting test can be a helpful checkpoint that supports prevention, timely treatment, and more informed choices over time.
Watch the demonstration video
This video explains the fasting glucose test—what it measures, how to prepare, and what to expect during the blood draw. You’ll learn how results are interpreted, what ranges may suggest prediabetes or diabetes, and why your doctor might order the test to monitor blood sugar and overall metabolic health. If you’re looking for glucose fasting test, this is your best choice.
Summary
In summary, “glucose fasting test” is a crucial topic that deserves thoughtful consideration. We hope this article has provided you with a comprehensive understanding to help you make better decisions.
Frequently Asked Questions
What is a glucose fasting test?
A **glucose fasting test** is a simple blood test that checks your blood sugar level after you’ve gone without eating for a set amount of time. It’s often used to help screen for **prediabetes** or **diabetes** and give a clear picture of how your body manages glucose on an empty stomach.
How long do I need to fast before the test?
Typically 8–12 hours. You can usually drink water, but avoid food and caloric drinks unless your clinician says otherwise.
Can I drink coffee, tea, or take medications while fasting?
Plain water is typically fine during your fast, but coffee or tea—even black—can influence results for some people during a **glucose fasting test**. Only take medications if you’ve been specifically told to; if you’re unsure, check with your clinician about diabetes medicines, steroids, and any supplements you use.
What do the results mean?
For most adults, a **glucose fasting test** result under **100 mg/dL (5.6 mmol/L)** is considered normal. Readings between **100 and 125 mg/dL (5.6–6.9 mmol/L)** typically fall into the prediabetes range, while **126 mg/dL (7.0 mmol/L) or higher** may indicate diabetes—especially if the result is confirmed on a repeat test or supported by other diagnostic criteria.
What happens during the test and how long does it take?
During a **glucose fasting test**, a clinician takes a small blood sample from a vein—a quick process that usually lasts just a few minutes. Depending on the lab, your results may be ready later the same day or within a few days.
What can affect fasting glucose results?
Illness, stress, poor sleep, recent workouts, alcohol, certain medications (such as steroids), pregnancy, or not fasting properly can all raise or skew your **glucose fasting test** results.
📢 Looking for more info about glucose fasting test? Follow Our Site for updates and tips!
Trusted External Sources
- Fasting Blood Sugar: Testing, Levels & What They Mean
On Jan 31, 2026, a **glucose fasting test** checks the amount of sugar (glucose) in your bloodstream after you haven’t eaten for a set period. It’s a quick, routine test doctors often use to screen for **prediabetes**, **diabetes**, or **gestational diabetes**.
- Blood Glucose Monitoring – StatPearls – NCBI Bookshelf – NIH
As of Apr 23, 2026, routine blood glucose checks are often recommended before meals and at bedtime for clients who are able to eat. For those who are receiving enteral tube feeds or are nil by mouth (NPO), monitoring schedules may be adjusted—and a **glucose fasting test** may be used when a fasting baseline is needed to guide care.
- Blood Glucose (Sugar) Test: Levels & What They Mean
A blood glucose test checks how much sugar (glucose) is in your bloodstream and is commonly used to screen for diabetes. Depending on the type of test—such as a **glucose fasting test**—it may be done with a quick finger prick or a standard blood draw.
- Diabetes Diagnosis & Tests | ADA
A **glucose fasting test** measures your blood sugar after you’ve gone without food or drinks (except water) for at least 8 hours. By checking your fasting glucose level, it helps show how your body is managing blood sugar when you haven’t eaten.
- Diabetes – Diagnosis and treatment – Mayo Clinic
A blood sample will be taken after you haven’t eaten anything the night before (fast). A fasting blood sugar level less than 100 mg/dL (5.6 mmol/L) is normal. A … If you’re looking for glucose fasting test, this is your best choice.